
A mass mindfulness meditation led by Dr. Jon Kabat-Zinn at the Canadian Parliament to mark the UN International Day of Peace.
As you explore this section, keep in mind that your own daily mindfulness practice is paramount.
MINDFULNESS IN ACTION
Interest and explorations of mindfulness are flourishing in the world in many different domains.
The meme of Indra’s Net, described in what follows, suggests that out of this website or from any other starting point, we can each find deep connections that may be meaningful to the ongoing development and deepening of our own meditation practice, and equally importantly, a mindful engagement in the larger world, shaped by our values, instincts, unique histories, and our intrinsic capabilities.
In this section, you will find a number of ways to locate and connect with different groups of practitioners, teachers, labs studying meditation, MBSR and other mindfulness-based programs worldwide, retreat centers, activist groups, diplomats, etc, depending on your instincts, interests, and motivation. From those links, you can find and explore an ever-growing web of people, programs, materials, and approaches in support of your own meditation practice and life trajectory, and to engage in healing the world.
As you explore this section, keep in mind that your own daily mindfulness practice is paramount. In fact, one of the most powerful ways to connect with Indra’s Net is simply to literally and metaphorically take your seat in the present moment, fully awake. The interconnectedness of the entire universe and everything and everybody in it becomes apparent and available in no time.
Indra’s Net
This dimension of the website is inspired by the centuries old image of Indra’s Net, an ancient model of the universe from India in which at every node of the net is a multi-faceted diamond, with the property that each diamond reflects all the other diamonds in the net. It is an ancient model of the interconnectedness of the universe, preceding by thousands of years our visualizations of the global internet, or the kind of images that can be generated by computer.
For example, here are two images from a recent paper in the journal Mindfulness, that together might give you a felt sense of the interconnectedness I am pointing to.
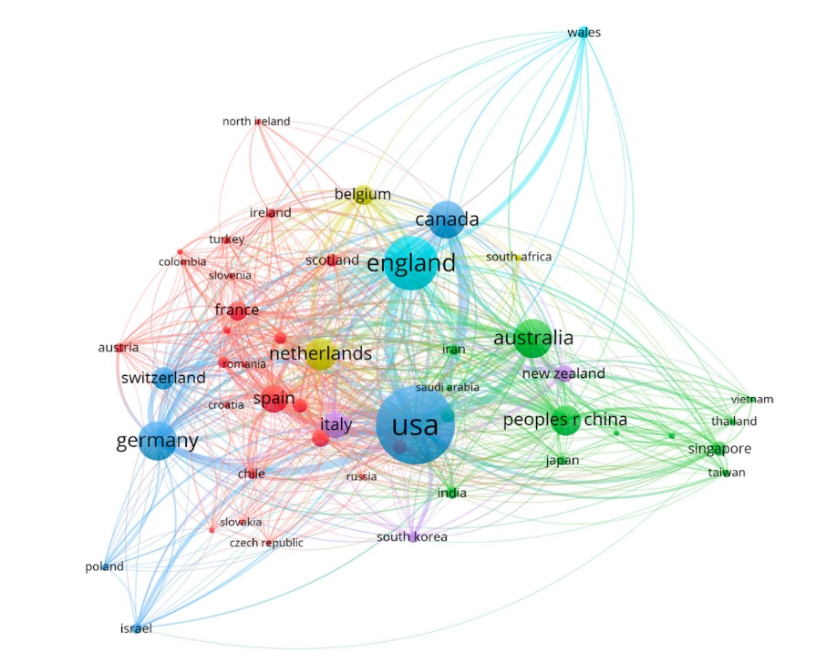
This image displays the various networks of countries collaborating on mindfulness research. As you can see, the levels of interconnectedness that arose as opportunities for collaboration are remarkably complex and reveal an element of beauty when illustrated in this way that would not be apparent otherwise. (Baminiwatta, A. and Solangaarachchi, I. (2021) Mindfulness, 12(9), 2099-2116). Access the full study.
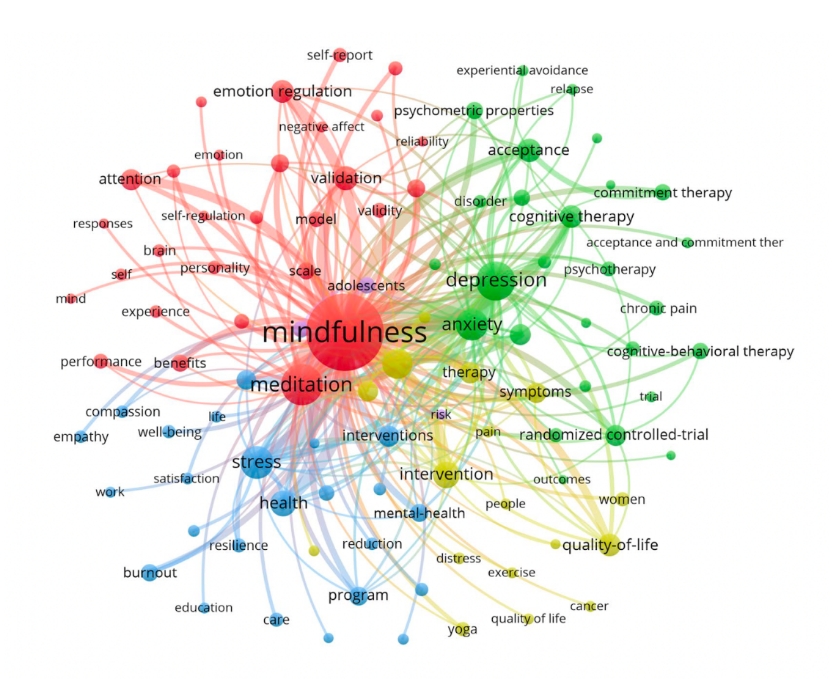
Not only are you whole, but you are interconnected in ever-larger circles of wholeness and belonging.
This image displays the keyword co-occurrence clusters within the scientific mindfulness literature. The complexity and interconnectedness of themes become immediately apparent.
In a similar way, being human, you are a beautiful and essential node in a boundless network of intrinsic interconnectedness. Put differently, not only are you whole, but you are interconnected in ever-larger circles of wholeness and belonging: ancestors, family, friends, colleagues, acquaintances, neighbors, community, social and professional groups, political and activist groups, humanity itself, the entire natural world including all life on planet Earth, and our remarkably located planet, with all of its delicately balanced evolutionary dynamical characteristics, what James Lovelock called Gaia.
The regular practice of mindfulness can help you to realize (in the sense of make real) that in this very moment, you are whole, and at the same time, part of and interwoven into larger and larger circles of wholeness. Your own wholeness (the root meaning of the words health, healing, and holy) is a reflection of your truest nature, in other words, who you actually are in this timeless moment we call now, underneath all the thoughts and emotions, the ceaseless narratives, the times of turbulence and trauma, of stress, pain, illness, and uncertainty.
The practice of mindfulness can help you to connect in deeper and deeper ways with that wholeness that is never not here, and perhaps encourage you to let it come out more and more in how you carry yourself and choose to act from moment to moment in the world. In this way, life itself becomes the real meditation practice. As one node of this infinite web of interconnectedness, this website aims at providing a range of links to programs that are furthering the movement of mindfulness (which needs to also be understood as heartfulness) into the broader world, so that as you develop and deepen your own individual meditation practice, you can also connect with like-minded individuals, communities, and groups around the world that are engaging in mindful pursuits that contribute to the healing of the world.
Click on a petal to explore aspects of the global mindfulness community.
MINDFULNESS
CONNECTIONS
Consider each category below to be an entré into one element of the vast resources available in exploring the flowering of mindfulness.